In this quick, easy-to-understand lesson, we learn about secondary hypertension for USMLE and medicine. Secondary hypertension is defined as high blood pressure (>140/90 or >130/80) caused by an underlying disease, medical condition, or drugs. While primary hypertension comprises of the majority of hypertension cases (90%), only 10% of patient cases is secondary hypertension.
Primary Hypertension vs Secondary Hypertension: What is primary hypertension? Read our first primary essential Hypertension USMLE lesson here to learn about the differences between primary hypertension and secondary hypertension.
There are many different causes of secondary hypertension, including chronic kidney disease, obstructive sleep apnea, NSAIDS drugs, among many.
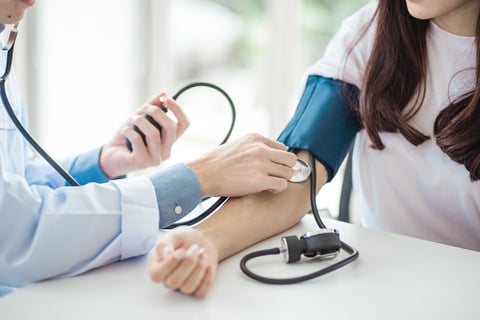
Determinants of Blood Pressure
Health Effects of High Blood Pressure
Blood Pressure = Cardiac Output x Total Peripheral Resistance
BP = CO x TPR
Bloor pressure can increase by either increased cardiac output (CO) or increased total peripheral resistance (TPR).
Cardiac Output on Blood Pressure
An example of increased cardiac output causing high blood pressure is increased renal salt and water retention. When more salt and water is retained in your body, cardiac output increases.
Total Peripheral Resistance
Remember that arterioles are the blood vessels with the highest resistance. Therefore, arterioles play a major role in affecting total peripheral resistance. When arterioles are constricted by vasoconstrictors (catecholamines), TPR increases. The sympathetic nervous system can also increase TPR.
TPR: arterioles (Increase by vasoconstrictors or Increase by sympathetic nervous system)
Chronic Kidney Disease
Over 80% of patients with chronic kidney disease have hypertension. Why? In chronic kidney disease, kidneys are not working well and specifically cannot excrete sodium well. Thus, there is higher sodium retention. Chronic kidney disease can also cause increased renin-angiotensin-aldosterone activity and sympathetic nervous system activity, which both can increase hypertension.

Obstructive Sleep Apnea
Sympathetic nervous system is ramped up because of sleep apnea, leading to hypertension.
NSAIDS on Hypertension
Drugs that cause secondary hypertension. NSAIDS: like ibuprofen, anproxen, indomethacin, ketorolac, diclofenac. NSAIDS are known as Nonsteroidal anti-inflammatory drugs. NSAIDS inhibit cyclooxygenase (COX) in kidneys. Cycloxygenase is an enzyme that converts arachidonic acid into prostaglandins. When cyclooxygenase is inhibited by NSAIDS, there is decreased synthesis of prostaglandins. PGE-2 plays a specific role in renal vasodilation in afferent arterioles. , so decreased PGE-2 can lead to hypertension. PGE-2 Afferent arteriole vasoconstricts, reducing renal blood flow and glomerular filtration rate, deceasing sodium/water excretion, and leading to hypertension.
NSAIDS –| (inhibit) Cyclooxygenase –> PGE-2
Decreased PGE-2 –> Vasoconstriction in afferent arteriole –> Decreased renal blood flow + Decreased Glomerular Filtration Rate –> Hypertension
Oral Contraceptive Pills that cause secondary hypertension
Estrogen and progesterone increase blood pressure
Hypertension: Causes and Health Effects of High Blood Pressure
Pseudoephedrine can cause Secondary Hypertension
Pseudoephedrine is a nasal decongestant and alpha-1 agonist. Its molecular structure is similar to epinephrine. Epinephrine constricts blood vessels in the nasal passage. Likewise, pseudoephedrine constricts blood vessels in the nasal passage. Vasoconstriction –> leads to decreased nasal blood flow.
Some of you may be thinking, “Wait, doesn’t epinephrine cause vasodilation?” Well, you’re not wrong. Epinephrine causes both vasodilation and vasoconstriction. Specifically, vasodilation for skeletal muscle via B2 receptor, and vasoconstriction in skin and kidneys and the nasal passage via Alpha-1 receptor!
Cyclosporine and Tacrolimus
Immunosuppressants
Calcineurin inhibitors and cause renal vasoconstriction because of salt/water retention. The best drug to treat hypertension yet still treats the same conditions is diltiazem, which treats hypertension and still has equally good efficacy for lower dose cyclosporine.
Click and check out these popular articles for more information: 🙂
Hypertension: Causes and Health Effects of High Blood Pressure
Circulatory System: Blood Flow Pathway Through the Heart
Circulatory System: Heart Structures and Functions
Ductus Arteriosus Vs Ductus Venosus Vs Foramen Ovale: Fetal Heart Circulation
Cardiac Arrhythmias: Definition, Types, Symptoms, and Prevention
Upper Vs Lower Respiratory System: Upper vs Lower Respiratory Tract Infections
Seven General Functions of the Respiratory System
Digestive System Anatomy: Diagram, Organs, Structures, and Functions
Kidney Embryology & Development: Easy Lesson
Psychology 101: Crowd Psychology and The Theory of Gustave Le Bon
Copyright © 2022 Moosmosis Organization: All Rights Reserved
All rights reserved. This essay first published on moosmosis.org or any portion thereof may not be reproduced or used in any manner whatsoever
without the express written permission of the publisher at moosmosis.org.

Please Like and Subscribe to our Email List at moosmosis.org, Facebook, Twitter, Youtube to support our open-access youth education initiatives! 🙂












Timely review for hypertension 🙂
LikeLiked by 1 person
Excellent article on blood pressure!
LikeLiked by 2 people
This is a really superb piece on hypertension. It certainly runs in many families and can be caused by secondary means as well.
LikeLiked by 2 people
Outstanding essay on high blood pressure and health effects! ❤
LikeLiked by 2 people
High blood pressure is silent and powerful at the same time. It can affect people before they know it. Excellent review article on blood pressure.
LikeLiked by 2 people
Wisely said. Thank you for sharing your insight!
LikeLiked by 1 person
high blood pressure is quite deadly
Stroke heart attacks etc
Those blood pressure meds are life savers even though I forget to take them sometimes 😂
Great article!!
LikeLiked by 1 person
Hope you enjoy the informational education article!
LikeLike
Superb article on hypertension.
LikeLiked by 1 person