Circulatory System: Blood Flow Pathway Through the Heart
In this quick easy-to-understand lesson, we learn about atrial fibrillation, causes, symptoms, diagnoses, and treatments for USMLE medicine.
Atrial fibrillation is the most common type of cardiac arrhythmia. This means the heart beat has an irregularly irregular rhythm. Normally, the order of the conduction through the heart is the following: SA node –> AV node –> His bundles –> Bundles Branches –> Purkinje Fibers. In atrial fibrillation, the conduction is disrupted as displayed in the images below.

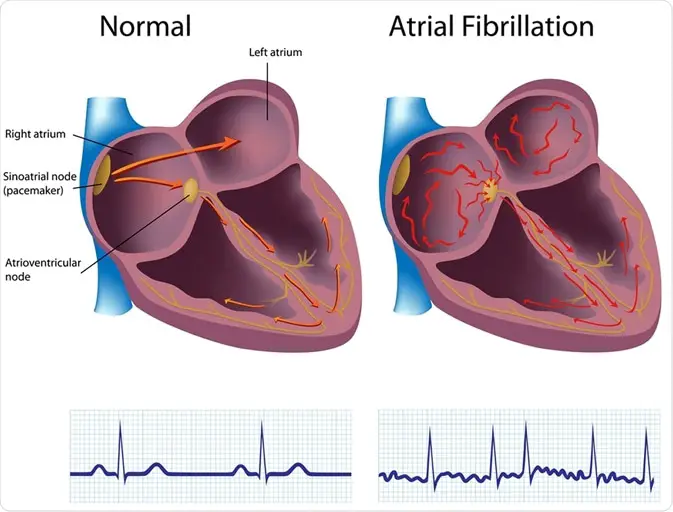
Depolarization occurs irregularly in many places in the atria. Some are refractory and do not go to the AV node, but some do, which then generates the resulting pulse. However, because we get hundreds of random depolarizations in the atria with some refractory and some passing to the AV node, the heart rhythm thus becomes irregular. This leads to atrial fibrillation.
Symptoms and Diagnosis of Atrial Fibrillation
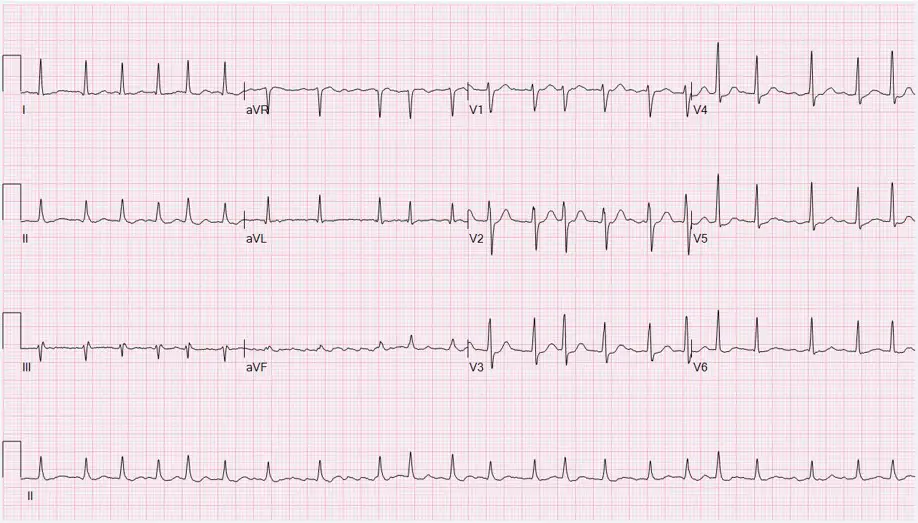
Symptoms can include fatigue, dyspnea (difficulty breathing), and heart palpitations in the chest. Atrial fibrillation can also cause syncope and fainting, leading to falls. You diagnose atrial fibrillation via EKG, such as in Figure 2 below. The EKG for atrial fibrillation lacks a P wave, labelled in a normal ECG in Figure 1.

ECG of Atrial Fibrillation
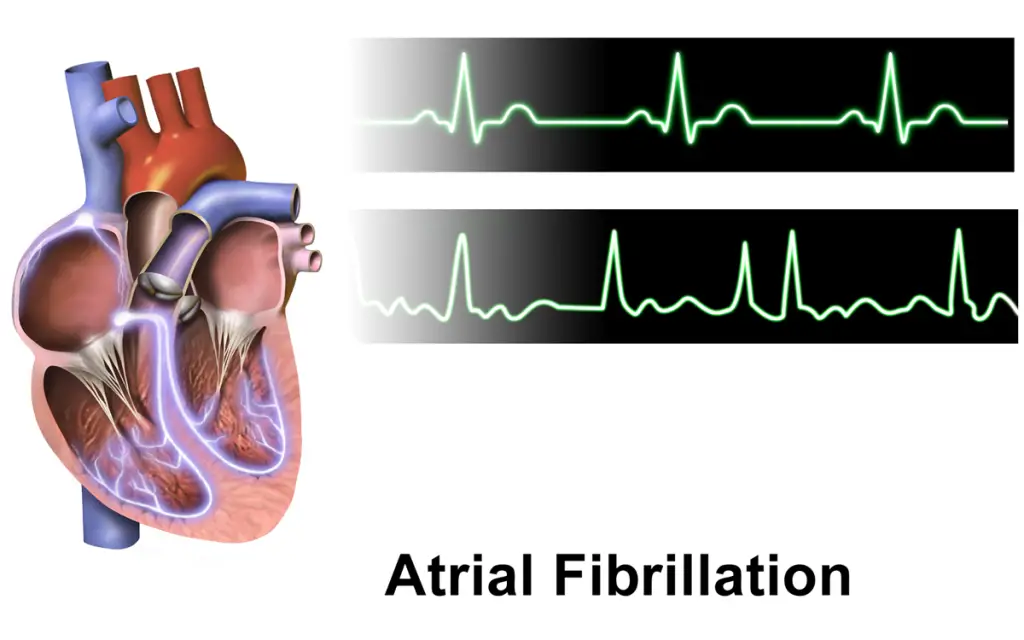
Types of Atrial Fibrillation
There are different types of atrial fibrillation: 1) Paroxysmal, 2) Persistent, and 3) Permanent.
Paroxysmal Atrial Fibrillation: this type of atrial fibrillation is spontaneous. Paroxysm literally means ‘violent outburst’ or ‘sudden attack.’ That is exactly what’s happening here. The heart’s rhythm may be irregularly irregular, but may spontaneously convert back to a regular sinus rhythm. The incidence of the atrial fibrillation is sudden, comes and goes, and can spontaneously convert back to a regular healthy rhythm of the heart, also known as sinus rhythm.
Persistent Atrial Fibrillation: this type of atrial fibrillation can last for days or weeks, much longer than just a spontaneous paroxysmal atrial fibrillation. For patients with persistent atrial fibrillation, they are often recommended a cardioversion treatment, which we will explain further down.
Permanent Atrial Fibrillation: this type of atrial fibrillation is permanent. Self-explanatory.
Asymptomatic Atrial Fibrillation: Patients with atrial fibrillation have a wide spectrum of symptoms. Not all patients will experience the same symptoms. Some patients are asymptomatic with heart rates <100 bpm, while other patients experience the classic symptoms palpitations, dyspnea, and fatigue with heart rates >100 bpm.
Asymptomatic / Heart rate <100 bpm
Palpitations, Dyspnea, Fatigue / Heart rate > 100 bpm
What Happens if We Won’t Treat Atrial Fibrillation?
If atrial fibrillation is not treated, the patient can face more severe health problems down the road. One problem that can occur if rapid atrial fibrillation is not treated is called “tachycardia-induced cardiomyopathy.” Tachycardia or fast heart rate can induce or cause cardiomyopathy, which can lead to systolic heart failure.
Atrial fibrillation can affect preload. Specifically, atrial fibrillation decreases preload. Why is that bad? When your heart contracts, the main starting electrical signal comes from your SA node. Then the signal travels to your AV node. It is here that the AV node refractory period determines your heart rate. During atrial fibrillation and because of the irregular signals to your AV node, ventricles are not filling enough before contracting. Preload decreases. This leads to hypotension and low cardiac output. This worsens for patients with aortic stenosis or diastolic heart failure and can enter shock.
Another problem for patients with atrial fibrillation is a thrombus in the left atrial appendage. There is very little blood flow in this appendage of the heart. If the thrombus (clot) breaks off and travels through the blood, it can cause a stroke (brain), mesenteric ischemia (gut), or splenic infarcts (spleen).
Valvular Atrial Fibrillation = associated with rheumatic heart disease (very high risk for thrombus)
Hyperthyroidism can lead to atrial fibrillation. You treat these conditions with therapy for the thyroid disease rather than using atrial fibrillation therapies. Diagnostic test: TSH levels in blood
Triggers and Causes of Atrial Fibrillation
Sometimes there is no cause or trigger of atrial fibrillation. Patients who binge drinking or have the ‘holiday heart’ can trigger atrial fibrillation. Surgery, severe pain, or infection can also trigger atrial fibrillation.
How Do We Treat Atrial Fibrillation? : Medications
Treatment for Atrial fibrillation. There are 3 arms of atrial fibrillation treatment: 1) heart rate, 2) heart rhythm, and 3) anticoagulation. For heart rate, we want to control the rate of the heart. This means slowing down the heart rate to ideally <110 bpm with beta-blockers, calcium channel blockers, or digoxin. These drugs slow AV node conduction.
Rate Control for Atrial Fibrillation: Treat with drugs that slow down the heart rate (specifically AV node conduction)
Beta blockers: b1 selective agents, metoprolol, atenolol
Calcium channel blockers: verapamil, diltiazem
Digoxin: increases parasympathetic tone
For heart rhythm treatment of atrial fibrillation, we want to make the heart beat regularly, not irregularly. This is done by taking anti rhythmic drugs to restore sinus rhythm or having patients undergo a cardioversion.
For all patients whether treated through 1) heart rate control or 2) heart rhythm control, we give them anticoagulants to reduce risk of thrombus.
What is Cardioversion Treatment for Atrial Fibrillation?
Cardioversion can be either electrical or chemical based. In electrical cardioversion, an electrical shock is delivered to the chest. This causes all the heart cells depolarize at the same time and hopefully causes the heart to become more synchronized. In chemical cardioversion, we administer antiarrhytmic medication.
Antiarrhytmic medications include Class I (flecainide and propafenone) and Class III 9amiodarone, sotalol, dofetilide)
Can atrial fibrillation go away by itself without any treatment? Yes, for some patients, atrial fibrillation spontaneously undergoes cardioversion by itself, meaning the heart returns to sinus regular rhythm.

Surgical Treatments for Atrial Fibrillation
Surgical therapy for atrial fibrillation include 1) pulmonary vein isolation (targeting some myocytes near the pulmonary veins at the entrance of the left atrium) and 2) atrial flutter ablation (targeting the right atrium).
Click and check out these articles for more information: 🙂
Circulatory System: Blood Flow Pathway Through the Heart
Circulatory System: Heart Structures and Functions
Ductus Arteriosus Vs Ductus Venosus Vs Foramen Ovale: Fetal Heart Circulation
Cardiac Arrhythmias: Definition, Types, Symptoms, and Prevention
Copyright © 2022 Moosmosis Organization: All Rights Reserved
All rights reserved. This essay first published on moosmosis.org or any portion thereof may not be reproduced or used in any manner whatsoever
without the express written permission of the publisher at moosmosis.org.

Please Like and Subscribe to our Email List at moosmosis.org, Facebook, Twitter, Youtube to support our open-access youth education initiatives! 🙂










Awesome article! My grandma has AFib and she just got treated for it!
LikeLiked by 1 person
Excellent facts! I learned something new today 🙂
LikeLiked by 1 person
Hope your Grandma’s doing well now, Samantha! Thank you for your kind comment! 🙂
LikeLiked by 1 person
Superb👍 love it ❤️
LikeLiked by 1 person
Excellent points about arrhythmias and atrial fibrillation!
LikeLiked by 2 people
Great essay on AFib.
LikeLiked by 2 people
Brilliant! —my cardiology doctor diagnosed atrial fibrillation for me
LikeLiked by 2 people